Appendicitis: Comprehensive Medical Guide to Symptoms, Diagnosis, Treatment and Recovery
A clear, clinician-informed overview of appendicitis — how it develops, how doctors diagnose it, the treatments (including when surgery is needed), recovery expectations and how to reduce risks.
Introduction
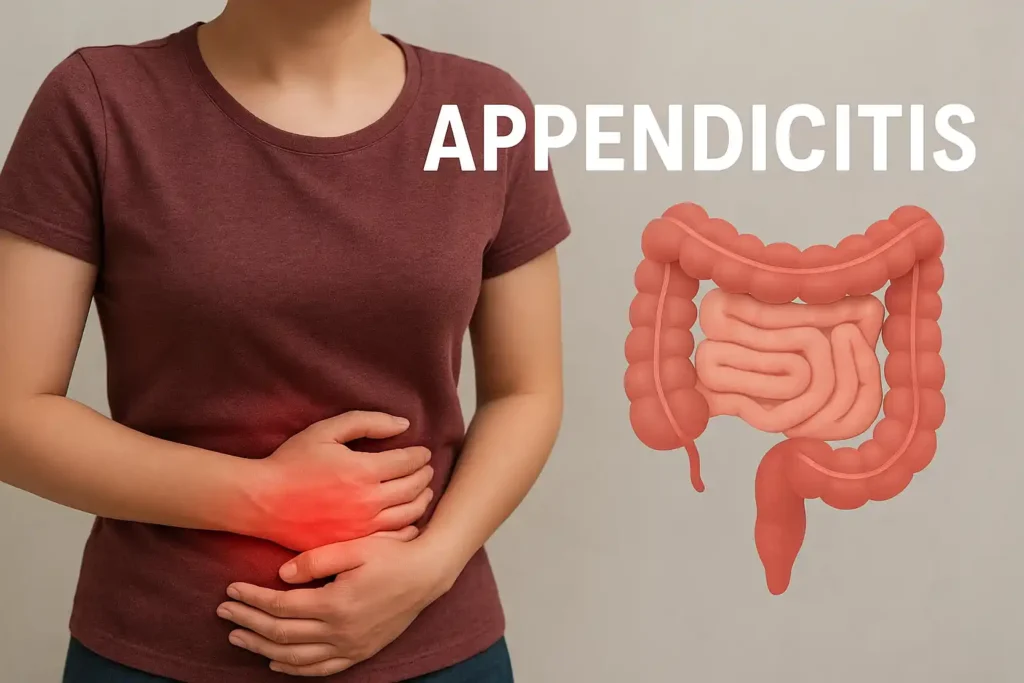
Appendicitis is an inflammation of the appendix, a small finger-shaped pouch attached to the large intestine. It is a common cause of acute abdominal pain that often requires prompt medical attention. Left untreated, an inflamed appendix can rupture, leading to serious infection in the abdominal cavity (peritonitis) or an abscess.
This guide explains the typical causes, the classic and atypical symptoms, the diagnostic tests clinicians use, treatment options (including non-operative management and appendectomy), the expected recovery timeline, potential complications, and practical advice for patients and families.
Anatomy and function of the appendix
The appendix is a narrow, tube-like organ about 6–10 cm long, attached to the cecum at the junction of the small and large intestines in the lower right abdomen. Historically considered vestigial, recent research suggests it may play a role in immune function and maintaining gut flora. Regardless, people live normally after appendectomy.
What causes appendicitis?
Appendicitis most often results from obstruction of the appendix lumen (the inside of the appendix). Common causes of obstruction include:
- Fecaliths (hard stool): the most frequent cause in adults.
- Lymphoid hyperplasia: swelling of lymphatic tissue (more common after viral infections or in children).
- Foreign bodies: rarely, seeds or other swallowed material.
- Parasites or tumors: unusual causes.
Obstruction leads to increased pressure, compromised blood flow, bacterial overgrowth and inflammation. If untreated, the inflamed appendix may rupture within 24–72 hours in many patients.
Symptoms: classic and atypical
Classic presentation
Typical appendicitis progression in adults:
- Periumbilical pain: sudden, poorly localized pain near the navel that begins first.
- Migration to right lower quadrant (RLQ): over 6–24 hours the pain typically shifts to the RLQ (McBurney’s point).
- Associated symptoms: anorexia (loss of appetite), nausea, vomiting, low-grade fever, constipation or diarrhea.
Atypical or variable presentations
Not everyone has the classic pattern. Symptoms vary by age, pregnancy, and position of the appendix:
- Children: may present with fever and diffuse abdominal pain; diagnosis can be harder.
- Older adults: may have milder pain but higher risk of perforation at presentation.
- Pregnancy: the growing uterus can displace the appendix, shifting pain higher in the abdomen.
- Retrocecal appendix: pain may be less localized and mimic back or flank pain.
Because of variability, any progressive abdominal pain with concerning signs should prompt medical evaluation.
When to seek emergency care (red flags)
If someone has abdominal pain that is intense, worsening quickly, or associated with any of the following, seek urgent medical attention or go to the emergency department:
- Severe, increasing abdominal pain
- Fever over 38°C (100.4°F)
- Inability to pass gas or stool with severe pain
- Vomiting that prevents keeping fluids down
- Signs of sepsis: very rapid heartbeat, low blood pressure, confusion
How is appendicitis diagnosed?
Diagnosis combines clinical evaluation, laboratory tests and imaging. No single test is perfect — clinicians synthesize findings.
Clinical examination
Key exam findings include:
- Tenderness at McBurney’s point: RLQ tenderness located two-thirds between the navel and the right anterior superior iliac spine.
- Guarding and rebound tenderness: signs of peritoneal irritation.
- Rovsing’s sign, psoas sign, obturator sign: physical maneuvers that may indicate appendiceal irritation depending on appendix position.
Laboratory tests
- Complete blood count (CBC): often shows elevated white blood cell (WBC) count with left shift (neutrophilia), but it can be normal early on.
- C-reactive protein (CRP): an inflammatory marker that may be elevated.
- Urinalysis: used to exclude urinary causes (e.g., urinary tract infection or kidney stone).
Imaging
Imaging helps confirm diagnosis and plan management:
- Ultrasound: first-line for children and pregnant patients — can show a non-compressible, enlarged appendix.
- CT scan (abdomen/pelvis with contrast): the most accurate imaging in adults; identifies inflammation, abscess, or perforation.
- MRI: an alternative in pregnancy when CT radiation is a concern.
Treatment options
Treatment depends on whether the appendix is inflamed without rupture (uncomplicated) or ruptured/complicated (perforation, abscess). Options include non-operative antibiotic therapy and appendectomy (surgical removal).
1. Appendectomy (surgical removal)
Appendectomy is the definitive treatment. There are two main approaches:
- Laparoscopic appendectomy (minimally invasive): small incisions, camera-guided removal, faster recovery, less postoperative pain and lower wound infection rates.
- Open appendectomy: single larger incision — used when laparoscopy is not available or when there is a complicated infection or extensive scar tissue.
Surgery is often performed urgently once the diagnosis is confirmed to reduce the risk of rupture. Many centers provide intravenous antibiotics prior to surgery.
2. Non-operative (antibiotics-first) management
Recent studies suggest that selected patients with uncomplicated appendicitis may be treated initially with antibiotics alone. Key points:
- Effective in many patients, but recurrence risk exists (some patients require appendectomy later).
- Best suited to carefully selected cases, with close follow-up and availability of surgery if condition worsens.
- Antibiotic selection typically covers common gut bacteria (e.g., broad spectrum covering gram-negative rods and anaerobes).
3. Managing complicated appendicitis (abscess or perforation)
If the appendix has ruptured and an abscess formed, options include:
- Percutaneous drainage: image-guided (CT/US) drainage of abscess followed by antibiotics, with interval appendectomy sometimes planned.
- Emergency surgery: laparoscopic or open washout and appendectomy if peritonitis or unstable patient.
What to expect during appendectomy
Preoperative: fasting, blood tests, IV antibiotics and fluids as needed, informed consent.
Anesthesia: general anesthesia for most patients.
Operative time: typically 30–90 minutes depending on complexity.
Postoperative: monitoring in recovery; pain control; early mobilization; resume diet gradually.
Length of stay depends on procedure and complication status — many elective laparoscopic cases go home same day or within 24 hours; complicated cases may require several days in hospital.
Recovery and follow-up
Immediate recovery (first week): pain and mild fatigue are common; avoid heavy lifting; follow wound care instructions; take antibiotics if prescribed.
2–4 weeks: most patients resume normal activities; wounds heal; return to work or school typically in 1–2 weeks depending on job demands.
Long-term: most people recover fully after appendectomy with no lasting effects. Watch for fever, increasing pain, wound redness or drainage — these may indicate infection and require evaluation.
If managed with antibiotics only: follow-up imaging or clinical checks are common, and patients should be educated on recurrence signs (recurrent RLQ pain, fever).
Possible complications
Complications are uncommon with timely care but include:
- Rupture/peritonitis — life-threatening if not treated
- Intra-abdominal abscess
- Surgical site infection
- Ileus (bowel slowdown) after surgery
- Adhesions causing future bowel obstruction (rare)
- Anesthesia-related complications
Special considerations: children, elderly and pregnancy
Children
Appendicitis is common in school-aged children and adolescents. Diagnosis can be more difficult; rapid progression to rupture is possible, so clinicians often have a low threshold for imaging and surgical consultation.
Elderly
Older adults may present atypically with milder pain but are at higher risk for delayed diagnosis and perforation. Comorbid conditions increase complexity in management.
Pregnancy
Appendicitis is the most common non-obstetric emergency in pregnancy. Imaging choices are guided by fetal safety (ultrasound first, MRI as alternative). Prompt surgical management is often recommended to minimize rupture risk.
Can you prevent appendicitis?
Specific prevention is not always possible because the exact trigger of obstruction is often unpredictable. Some observational studies suggest a high-fiber diet may reduce the risk of appendicitis by promoting regular bowel movements and reducing fecalith formation, but evidence is not conclusive.
General advice: maintain a healthy diet with adequate fiber, seek prompt evaluation for progressive abdominal pain, and treat gastrointestinal infections appropriately.
Practical tips for patients
- Do not self-medicate to mask severe abdominal pain: painkillers can hide worsening signs and delay diagnosis.
- Bring a list of medications and allergies to the ER.
- Ask about surgical approach: laparoscopic vs open and expected recovery timeline.
- Follow postoperative instructions: wound care, activity restrictions, and follow-up appointments.
- Watch for warning signs: fever, increasing pain, wound drainage, or new vomiting should prompt a return to care.
Frequently asked questions (FAQs)
Can appendicitis go away on its own?
Appendicitis rarely resolves without treatment. While some early, uncomplicated cases may respond to antibiotics, the risk of recurrence or rupture exists. Always seek medical evaluation for suspected appendicitis.
How long after appendectomy can I return to work?
After a laparoscopic appendectomy, many people return to light duties in 1–2 weeks and normal activities by 4 weeks. Open surgery or complicated cases may require longer recovery. Follow your surgeon’s guidance.
Is laparoscopy always better?
Laparoscopic surgery often offers faster recovery and less pain, but the choice depends on clinical factors (e.g., rupture, abscess, previous surgeries) and surgeon expertise.
References & further reading
This article summarizes commonly accepted clinical guidance. For patient-facing references consider resources from: the American College of Surgeons (ACS), American Academy of Pediatrics, National Institutes of Health (NIH), and UpToDate (for clinicians).